Work-Related Eye Injuries – Examples
There is a wide range of ways that you could injure your eyes at your work place. Some are quite obvious, while others occur while you least expect it.
Here are some examples of work-related eye injuries:
Chemical eye burns
Both highly acidic and highly alkaline substances are toxic to the eye and can cause chemical eye burns if they come into contact with the surface of the eye. Alkaline substances present the greatest risk. Such substances are most commonly found in the workplace, for example in laboratory chemicals or industrial cleaning products.
Invasion of foreign bodies
The eye may sometimes get invaded by small foreign particles such as dust from manufacturing activities, which can cause irritation and inflammation. While foreign particles rarely cause lasting damage to the eyes, removal of irritating particles is necessary to avoid permanent eye damage.
Blunt trauma injuries
Blunt trauma injuries (i.e. injuries which do not penetrate the skin and do not result in external bleeding) to the eye occur as a result of being struck by a heavy object. They can cause the eye to bleed internally.
Allergic conjunctivitis
Allergic conjunctivitis is common amongst workers in food handling and agricultural lines of work, who are regularly exposed to particular spices, fruits and vegetables. Excessive exposure to ultraviolet radiation such as sunlight is associated with working in an outdoor industry and also increases risk of allergies.
Eye diseases associated with ultraviolet radiation exposure
Outdoor workers are often exposed to ultraviolet radiation in the form of sunlight in excessive quantities. There are numerous eye diseases and disorders associated with the eyes’ exposure to ultraviolet radiation. Outdoor workers have an increased risk of developing these conditions.
Artificial sources of ultraviolet radiation are also found in a range of workplaces and is also damaging to the eyes. These include welding arcs, germicidal lamps and lasers.
Computer use disorders
Using a computer for extended periods of time is associated with a range of temporary eye disorders including pain and altered vision.
WPBF 25 Dr. Oz Health & Wellness Festival 2015
Join Us! At the Palm Beach Gardens mall this saturday and visit the Rand Eye Institute’s booth for the Annual WPBF 25 Dr. Oz Health & Wellness Festival 2015.
WPBF 25 Dr. Oz
Health & Wellness Festival 2015
Saturday, March 28th
10AM – 4PM
Location: The Gardens Mall
3101 PGA Boulevard
Palm Beach Gardens, FL 33410
Dr. Oz will be bringing his exciting health show LIVE to the Gardens Mall with 2 NEW must hear presentations!
Lisa Oz, best-selling author, show host and editor of Dr. Oz’s magazine The Good Life, joins her husband on stage! She will be presenting her holistic family medicine and will provide tips on how to cook healthier versions of some of your favorite dishes.
Visit the Rand Eye Institute’s booth, at the Dr. Oz Health and Wellness Festival, and enter our raffle giveaway for a chance to win one of 2 Spa finder gift cards. The winner will be drawn at the end of the Health and Wellness Festival. You do not need to be present to win. Only 1 entry per person. Some restrictions apply.* 18 years or older to enter. *
THIS IS A FREE OPEN TO THE PUBLIC EVENT.
Workplace Eye Safety Tips – Checklist
Eye injuries in the workplace are very common. More than 2,000 people injure their eyes at work each day. About 1 in 10 injuries require one or more missed workdays to recover from. Of the total amount of work-related injuries, 10-20 % will cause temporary or permanent vision loss.
Here’s a quick checklist to help avoid workplace eye injuries:
Workplace Eye Safety Checklist:
Create a safe work environment.
- Minimize hazards from falling or unstable objects.
- Make sure that tools work and that safety features are in place.
- Make sure people know how to use tools properly.
- Keep bystanders out of hazardous areas.
- Evaluate safety hazards.
- Identify the primary hazards at the site.
- Identify hazards from nearby workers, large machinery, and falling/shifting objects.
- Wear the proper eye and face protection.
- Select the right eye protection for the work site.
- Make sure safety eyewear is in good condition.
- Make sure safety eyewear fits right and stays in place.
- Use smart workplace safety practices.
- Always brush, shake, or vacuum dust and debris from hardhats, hair, forehead, or your brow before removing protective eyewear.
- Don’t rub eyes with dirty hands or clothing.
- Clean eyewear regularly.
Most workplace injuries occur where safety eyewear isn’t required, or left up to the individual to decide if they’ll wear it. Many of those injured on the job didn’t think they needed to wear protective gear, or were wearing eyewear that didn’t provide adequate protection. Most work place injuries occur where safety eyewear isn’t required, or left up to the individual to decide on wearing. Many of those injured on the job did not think they needed to wear protective gear, or were wearing the wrong type of eyewear that did not offer adequate protection.
Living with Age-Related Macular Degeneration
How to Improve your Daily Life When Having (AMD) Age-Related Macular Degeneration
If you are losing your sight, there are some things you can do to improve your vision and live more comfortably.
Millions of people live with macular degeneration and they continue to complete their daily tasks as they always have.
Lighting-
Good lighting can make a big difference, especially if you are planning on performing a task that requires attentive sight, such as reading a book or knitting. Having good lighting also creates a safer environment and helps prevent accidents.
Having too much or too little light can be dangerous for a person with low vision. Testing out different kinds of lights and their levels can help you determine which you are most comfortable seeing with.
Computers-
Computers can be very valuable for people with low vision. It can help them perform their work, shop, bank and communicate with friends with more ease. Changing the settings on your computer can help with brightness and dimness, font size and much more.
Choosing the right pair of glasses is important in working well with computers. Distance glasses are designed to focus on objects at 20 feet. Reading glasses are designed to focus at 12 to 16 inches when you look down. Computer screens are generally positioned straight ahead at a distance of 20 inches from your eyes. Choose glasses that focus specifically on your computer screen. These glasses should also include a filter to reduce glare and reflections.
Driving-
Driving with low vision is extremely dangerous and should be avoided at all cost. If you do pass the Department of Motor Vehicles driving test, take precautions while operating a car.
Always wear your glasses.
Eating Right-
Although eating the right food cannot reverse maculate degeneration, it can help control and prevent it.
Eat a lot of fruits and vegetables: Antioxidants fight against oxidation, which is a part of the process of AMD. Consuming dark, leafy vegetables like kale, spinach, mustard greens and collard greens is great because it contains lutein, which is a critical antioxidant. Antioxidants are also found in fruits and vegetables with bright colors, such as red grapes, peppers, corn, oranges, cantaloupe and mango.
Eat Fish: People who eat fish 2-3 times a week have a much lower risk of developing AMD, because of the Omega-3. You can also get your Omega-3 intake by obtaining omega-3 supplements. Fish oil capsules are popularly chosen.
Limit Your Fat Intake: Research has shown that the real issue for AMD is the amount of saturated fats consumed in diets. The biggest source that people get comes from beef, pork, lamb, butter, whole milk, eggs, etc. Maintain your fat intake, by substituting them for something lower in fat.
Age-Related Macular Degeneration Types & Treatment
Types of Age-Related Macular Degeneration and How to Treat Them
There are two types of AMD: dry and wet. Both destroy the clear, see-straight central vision necessary for reading, driving, identifying faces, watching television and performing other daily activities. Peripheral vision may not be affected and it may be possible to see side views. Dry AMD About 90% of AMD cases are classified as dry Age-related Macular Degeneration. Usually, AMD starts as the dry type and can develop in one or both eyes. This process is slow and can advance over the course of several years, Many people do not even realize they have AMD, because early dry AMD is usually mild and free of symptoms.
Dry AMD has three stages:
- Early: In this stage, central vision is usually not affected. The eyes may have some small drusen, but there is a low risk of it progressing to advanced-dry AMD.
- Intermediate: In this stage, near and distance vision is affected, and a person may have a blind spot or blurring in the central vision. People with intermediate dry AMD are likely to have many medium-sized drusen, or one or more large drusen. After five years with intermediate dry AMD, the risk of it progressing toward the advanced stage is higher, but still low. For people with large drusen in both eyes, the risk of developing advanced AMD is greater.
- Advanced: At the advanced stage, the cells in the macula completely lose their ability to function. There is a definite blurred or blank spot in the centre of one’s sightline. Over time, vision will likely worsen and a person will have difficulty reading or recognizing faces. Up to 43 percent of people in this stage of dry AMD will progress to wet AMD, the more aggressive form of the disease.
Wet AMD
Wet Age-Related Macular Degeneration is the most severe form of AMD and can cause a sudden loss of vision within weeks or months. Recognizing and managing wet AMD early can asset in preventing further vision loss. Wet AMD involves the unexpected growth of abnormal blood vessels below the retina, which breaks into the macula causing blood and fluid to leak. Once wet AMD is presented in one eye, the chance of it developing in the second is greater.
Age-Related Macular Degeneration
What is the Macula?
The macula is made up of million of light-sensing cells that provide sharp, central vision. It is the most sensitive part of the retina. It is located at the back of the eye. The retina turns light into electrical signals and then sends these electrical signals through the optic nerve to the brain. There they are translated into images that we see.
What You Should Know….
 Age-related Macular Degeneration (AMD) is a common eye condition and a leading cause of vision loss among people age 50 and older. It is caused by damage to the macula. This can result in blurred, dark and distorted vision.
Age-related Macular Degeneration (AMD) is a common eye condition and a leading cause of vision loss among people age 50 and older. It is caused by damage to the macula. This can result in blurred, dark and distorted vision.
In some people, AMD advances slowly so vision loss does not occur for a long time. In other cases, the disease causes damage much faster and can lead to vision loss in one or both eyes.
Who is at Risk?
Age is a big factor for AMD. The disease is more likely to occur after the age of 60.
Other risk factors include:
- Smoking- Research has proven that smoking doubles the risk for AMD.
- Race- ADM is more common among Caucasians then African Americans or Hispanic/Latinos.
- Family History- People with a family history are at higher risk.
- Obesity- Being severely overweight increases the chance of developing AMD.
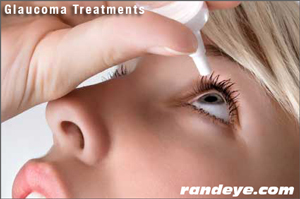
Glaucoma Treatments
Treatment for glaucoma depends on the nature and severity of each case. In general glaucoma cannot be completely cured, but it can be controlled. Most treatments for glaucoma are designed to reduce or control intraocular pressure (IOP), which can damage the optic nerve that transmits visual information to the brain. With any type of glaucoma, regular eye examinations are very important.
Glaucoma Modes of Treatment:
Medicine
Glaucoma is often treated with eye drops that are taken regularly several times a day. The eye drops help alter the circulation of the eye fluid and lower eye pressure, by either decreasing the production of fluid within the eye or by increasing the flow leaving the drainage angle. Because glaucoma can worsen over time without you being aware of it, your treatment will likely change in order to achieve a lower eye pressure.
Laser Surgery
Laser surgery is also effective for glaucoma treatment. Trabeculoplasty is a type of laser treatment that enhances eye drainage function to help control eye pressure within the eye when treating open-angle glaucoma. Iridotomy is a laser treatment that makes tiny holes in the iris to help improve the flow of eye fluid to the drain when treating narrow angle
Operative Surgery
If eye drops and laser therapy treatment have not been successful in lowering the eye pressure, your doctor might suggest operative surgery, where a new bypass drainage tunnel will be created using a microscope and specialized instruments, in order for the eye fluid to leave the eye.
Each case of glaucoma is different and treated differently. Talking to your doctor can help you distinguish which treatment is best for you.
Glaucoma Symptoms & Types
Glaucoma refers to a group of related eye disorders that all cause damage to the optic nerve that carries information from the eye to the brain. Glaucoma usually has few or no initial symptoms. 
In most cases, glaucoma is associated with higher-than-normal pressure inside the eye. But it also can occur when intraocular pressure (IOP) is normal. If untreated or uncontrolled, glaucoma first causes peripheral vision loss and eventually can lead to blindness.
Types and Symptoms of Glaucoma
Primary open-angle glaucoma. This common type of glaucoma gradually reduces your peripheral vision without other symptoms. By the time you notice it, permanent damage already has occurred. If your IOP remains high, the destruction can progress until tunnel vision develops, and you will be able to see only objects that are straight ahead. Ultimately, all vision can be lost, causing blindness.
Acute angle-closure glaucoma. Also called narrow-angle glaucoma, acute angle-closure glaucoma produces sudden symptoms such as eye pain, headaches, halos around lights, dilated pupils, vision loss, red eyes nausea and vomiting.
Normal-tension glaucoma. Normal-tension glaucoma is a type of open-angle glaucoma that can cause visual field loss due to optic nerve damage. But in normal-tension glaucoma, the eye’s IOP remains in the normal range. Also, pain is unlikely and permanent damage to the eye’s optic nerve may not be noticed until symptoms such as tunnel vision occur. The cause of normal-tension glaucoma is not known. Many doctors believe it is related to poor blood flow to the optic nerve. Normal-tension glaucoma is more common in those who are Japanese, are female and/or have a history of vascular disease.
Congenital glaucoma. This inherited form of glaucoma is present at birth, with 80 percent of cases diagnosed by age one. These children are born with narrow angles or some other defect in the drainage system of the eye. It’s difficult to spot signs of congenital glaucoma, because children are too young to understand what is happening to them. If you notice a cloudy, white, hazy, enlarged or protruding eye in your child, consult your eye doctor.
Glaucoma Awareness Month 2015
Glaucoma is a disease that damages the eye’s optic nerve. The optic nerve is connected to the retina and is made up of many nerve fibers; the optic nerve is responsible for sending signals from your retina to your brain, where these signals are interpreted as the images you see.
In a healthy eye, a clear fluid called aqueous humor circulates the front portion of your eye. To maintain a constant healthy eye pressure, your eye continually produces a small amount of aqueous humor while an equal amount of this fluid flows out of your eye. If you have glaucoma, the aqueous humor does not flow out of the eye properly. Fluid pressure in the eye builds up and, over time, causes damage to the optic nerve fibers.
If left untreated, Glaucoma can lead to vision loss and eventually blindness.
Glaucoma Risk Factors:
Age
People over 60 are at increased risk for the disease. African Americans have an increase risk begin at the age of 40. The risk of developing glaucoma increases with every year of age.
Ethnic background
African-Americans older than age 40 have much higher risk of developing glaucoma than do Caucasians. African-Americans also are more likely to experience permanent blindness as a result of glaucoma. People of Asian descent have an increased risk of developing acute angle-closure glaucoma. People of Japanese descent may be more likely to have normal-tension glaucoma.
Family history of glaucoma
If you have a family history of glaucoma, you have a greater risk of developing it. Glaucoma may have a genetic link, meaning there’s a defect in one or more genes that may cause certain individuals to be more susceptible to the disease. A form of juvenile open-angle glaucoma has been clearly linked to genetic abnormalities.
Medical conditions
Several conditions may increase your risk of developing glaucoma, including diabetes, heart diseases, high blood pressure and hypothyroidism. Previous eye injuries can also cause glaucoma.