Dry Eye Prevention Tips
The desert can be dry. Drinks can be dry. Jokes can be dry, but your eyes? That’s no laughing matter. They require a normal flow of moisture so they function properly for good vision and maximum comfort.
It’s Dry Eye Month, so here are four fab tips to help prevent dry eyes and give you more vision comfort here in the middle of summer.

- The easiest and fastest way to temporary dry eye relief is to pick up doctor recommended non-prescription artificial tears. These over the counter lubricating eye drops may help relieve dry eyes, though not permanently. Keep some handy in your purse or pocket for the times a day when you may need to refresh.
- A warm compress placed over the eye in the morning can wash out or melt the oily secretions blocking the flow of tears, which cause the eyes to feel dry. Just a face towel placed in warm water and held over the eye for 10 or 20 seconds, repeated a few times, may do the trick. If you find no relief then it’s definitely time to schedule an eye exam.
- Give up smoking. Smoking exposes your eyes to high levels of oxidative stress, plus dryness, smoke and heat. Smoking increases the risk of developing a variety of conditions that affect your eye health.
- Are punctal plugs an option for me? Ask your ophthalmologist-dry eye specialist about punctal plugs: tiny stoppers that control the flow of tears from your tear ducts. This is a simple in-office procedure that may bring great relief to your eyes.
Contact our Dry Eye Specialist Dr. Allison Rand at The Rand Eye Institute for more details and to schedule your next eye exam.
How We Treat Dry Eyes
Punctal Plugs
We have glands that produce tears, an aqueous solution or oil secretions, and then we have drainage ducts. At the nasal aspect of both upper and lower lids is a small hole, the beginning of a tube that drains from the eye to the nose. If your eyes are very dry, we insert a tiny polymer stopper into the drainage duct to block it. If we block the lower duct, we cut approximately 50% of the drainage, so the tears that are produced last longer on the surface of the eye instead of being drained through the nose. If the dry eye is very severe, we can block both the upper and lower punctum so that whatever tears produced will have more of an effect.

Artificial, preservative-free tears
We lose tears from drainage and evaporation. Artificial lubricating tears and gels are available to add moisture to dry eyes. To lubricate the eye, there are different types of solutions available. There are watery solutions, and we have gel solutions, which are thicker and last longer on the surface of the eye, but may slightly blur vision. We have ointments, which are a greasy petroleum gel-like supplement. Adding a warm compress in the morning washes the ointment out, providing additional relief.
Warm Compresses
Warm compresses stimulate the dilation of the oil pores and make the oily secretions more fluid, similar to when you melt butter with heat. With the oil secretions more fluid, they find the bigger drainage duct and drain, resulting in more oil on the lacrimal surface. We recommend using a washcloth placed in warm water to hold over the eyes for 10 to 20 seconds as it cools off. Reheat it and bring it back to the eye and apply for two to three minutes, so that enough warmth is able to relieve your dry eye symptoms.
A Guide to Dry Eye Prevention
There is no guaranteed treatment to prevent dry eyes, but with the supplementation of omega-3 fatty acids, found in flaxseed oil, salmon, some cereals, walnuts, basil, broccoli and grape leaves, symptoms can be better controlled. Omega-3 fatty acids help the oil secretion from the lid glands. With a healthier oil layer, the evaporation rate and the friction from blinking are less. Artificial tears can also help. If you stare at a computer screen for hours, your blinking rate is diminished. We recommend periodic breaks with the use of an extra drop of artificial tears.
Come See Us
If you feel that you are experiencing symptoms of Dry Eye, schedule a comprehensive eye exam with Dr. Allison Rand, our Dry Eye Specialist. Call 954-782-1700.
Article source: Gabriel E. Velazquez, MD, Academic Director at Rand Eye Institute
National Dry Eye Awareness Month
What Causes Dry Eyes?
Our tears serve a purpose, they are designed to provide much needed moisture to our eyes. Later in life, some of us can experience dry eyes, a condition in which the eyes do not provide the moisture we need.
Dry eye is a multi factorial disease. Sometimes it can occur if the immune system attacks the lacrimal glands and our eyes fail to produce enough tears. It also may be secondary to chronic inflammation of the lids, when the oil glands in the lids don’t produce enough oil. It can also be a combination of both.

Who is most Likely to Experience Dry Eyes?
Dry eye is a condition more commonly found in females, especially those who are post-menopausal. It can, however, be found in either gender, typically after the age of 50 and more commonly after age 65. It is important to know that dry eyes can occur at any age.
How You Can Tell if You Have Dry Eye
Symptoms include eye irritation or the sensation of a foreign body in the eye. You might experience discomfort after a few minutes of reading, and strangely enough, even watery eyes. Your eyes may sting or burn. You may experience dry eye in specific situations, such as on an airplane, in an air-conditioned room, while riding a bicycle, in an open convertible or after looking at a computer screen for an extended period of time.
How Could Watery Eyes be a Symptom of Dry Eyes?
It seems counterintuitive, but tearing can be a sign of dry eye. We have two kinds of tears: the basal secretion tears that keep the eyes lubricated, and reflex tears, which are watery and abundant. Normally, reflex tears occur after a stimulus, such as a grain of sand that becomes trapped in your eye. The natural defense of the ocular surface is to try to wash it out. It can also be a reflex to an emotional stimulus, such as crying because you’re sad or if you are slicing an onion. If you have insufficient basal secretion tears, and your eyes get irritated, this can stimulate reflex tears.
How Often We See Dry Eyes at Rand Eye Institute
Dry eye is very common. Most people who have had eye exams know that artificial tears are available. Many patients come to Rand Eye Institute for other reasons, but during the eye exam we may find they have dry eyes in addition to other conditions such as cataracts or glaucoma. Many patients may have had symptoms for awhile, but have not been diagnosed with dry eye until we examine them and connect their symptoms with the correct diagnosis.
Article source: Gabriel E. Velazquez, MD, Academic Director at Rand Eye Institute
Computer Vision Syndrome
As more of today’s workforce use computer monitors in the office, more often, workers are experiencing a new type of eye fatigue known as:
Computer Vision Syndrome
While there is no evidence that Computer Vision Syndrome causes any long-term damage to the eyes, regular computer use can be the source of significant eyestrain and discomfort.
If you have Computer Vision Syndrome, you may be experiencing some or all of these symptoms:

- Blurred vision
- Double vision
- Dry, red eyes
- Eye irritation
- Headaches
- Neck or back pain
Untreated, these symptoms can have a real effect on your work performance.
There is a way to relieve Computer Vision Syndrome just by making a few simple changes in your work environment.
Cut the glare
Changing the lighting surrounding your environment can reduce glare on your screen. Consider adding a movable shade to a nearby window. Lower the shade and move the monitor to the side slightly until the glare disappears. You might ask your employer to install a dimmer switch to the overhead lights, or add a desk lamp with a movable shade that distributes light evenly over your workspace. Adding a glare filter over your monitor screen can also help protect your eyes.
Rearrange your workspace
Research shows that the optimal position for your computer monitor is slightly below eye level, or about 20 to 28 inches away from the face. At this position, you should not have to stretch your neck or strain your eyes to see what’s on the screen. Use a copy stand to place any printed materials you may be working from on it so you don’t have to look up and down at the desk while you type.
Give your eyes a break
Look away from the screen every 20 minutes or so, gaze out the window or scan the room for about 20 seconds to rest your eyes to give them a chance to refocus and rest. Blink often to keep your eyes moist. If your eyes are dry, try using sterile lubricating eye drops.
Tweak your computer settings
Try adjusting the brightness, contrast and font size until you find the best settings for your vision. Most writing software programs have a percentage adjustment tab, commonly found at the very top center of your document that allows you to increase the font appearance temporarily and restore it when the document is complete.
Visit your eye doctor regularly for an exam, or schedule a comprehensive eye exam at The Rand Eye Institute. Let the doctor know about eyestrain or any other problems you might be experiencing at work. Call 800-782-1711
Diabetes Can Cause Vision Problems
People who do have diabetes have a higher risk for blindness than people without it.
Some of these vision problems include: 
Glaucoma
People with diabetes are 40% more likely to suffer from glaucoma than people without it. The longer someone has diabetes, the more common it is. Risk also increases with age.
Cataracts
Many people without diabetes get cataracts, but people with it are 60% more likely to develop them. People with diabetes also tend to get cataracts at a much younger age and have them progress faster. With cataracts the eyes clear lens cloud up and block light.
Retinopathy
Diabetic retinopathy is a term used for all disorders caused by diabetes. There are two major types of retinopathy: non-proliferative and proliferated.
Non-proliferative Retinopathy: Is the most common type of retinopathy. This occurs when capillaries in the back of the eye balloon up and form pouches. Non-proliferated retinopathy can move through three stages (mild, moderate and severe) as more blood vessels become blocked.
Proliferative: In this form, the blood vessels are so damaged they close off and new vessels start growing in the retina. These new vessels are very weak and can leak blood, blocking vision. The new blood vessels can also cause scar tissue to grow. After the scar tissue shrinks, it can distort the retina or pull it out of place.
If you notice any changes in your vision, an appointment with your eye doctor should be scheduled, immediately.
Vision and Eye Problems, That Tend to Arise While Aging
There are several eye problems that become increasingly common among people as they age:

-
Presbyopia:
This is the loss of ability to see objects close up, clearly. This includes small prints, as well. It is a normal process that happens slowly as you get older, but you will probably not notice a change in your vision until your 40s. Presbyopia can be corrected with reading glasses or contacts.
-
Floaters:
These are tiny specks or spots that float across your field of vision. Most people notice them while in a well-lit room or while outside. Floats are usually normal, but can sometimes indicate a more serious eye problem, such as retina detachment.
-
Dry eyes:
This happens when tears glands cannot make enough tears or they produce poor quality tears. Dry eyes can be uncomfortable, itchy, burning, redness and sometimes even some loss of vision.
-
Cataracts:
These are cloudy areas that cover part or the entire lens inside the eye. When a cataract is present, light can’t pass through the lens easily, and this causes vision to be impaired. If a cataract becomes too thick, they can be removed by surgery.
-
Glaucoma:
This develops when there is too much fluid pressure inside the eye. If this is not treated early, it can cause blindness or vision loss.
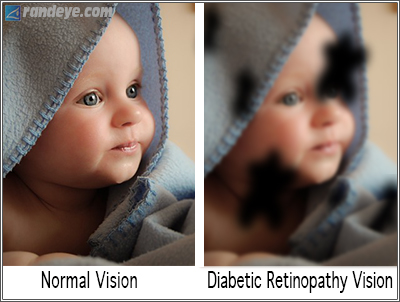
Diabetic Retinopathy – Diabetes
Diabetic Retinopathy
Is the most common complication of diabetes that affects the eyes and affects over 5.3 million Americans, 18 years old or older. It is caused by damage to the blood vessels of light-sensitive tissue at the back of the eye.
At first, diabetic retinopathy may cause no symptoms or only slight vision problems, however, eventually, it can result in blindness. Diabetic retinopathy can develop in anyone who has type 1 or type 2 diabetes. The longer a person has diabetes and the less controlled their blood sugar is, the higher at risk they are.
Symptoms include:
- Floaters
- Fluctuating vision
- Dark or empty areas in your vision
- Vision loss
- Difficulty with color perception
Patients with diabetes prevent or slow the development of diabetic retinopathy by taking prescribed medication as directed maintaining a healthy diet, exercising regularly, controlling high blood pressure and abnormal blood cholesterol levels, and avoiding alcohol and smoking. If the disease does develop, the potential for significant vision loss can be reduced by more aggressive blood sugar, pressure and cholesterol control. In addition, newer medications for retinopathy have recently been shown to be very effective for preserving, and sometimes improving vision.
There are several factors that can influence someone with diabetes to develop diabetic retinopathy. These include poor blood sugar, blood pressure and blood lipid control, the length of time they’ve had diabetes, race and family history. African Americans and Hispanics are twice as likely to have diabetes.
If you have diabetes, see your eye doctor for a yearly-dilated eye exam — even if your vision seems fine — because it’s important to detect diabetic retinopathy in the early stages.
Diabetic Eye Disease – Awareness Month
Diabetes is the leading cause of blindness in working-age Americans.
According to the American Academy of Ophthalmology, about 29 million Americans, 20 or older have diabetes and almost one-third does not even know they have the disease and are at risk for losing their vision.
Early symptoms of diabetes can often go undetected and vision may not be affected until the disease is more severe and even harder to treat. Some symptoms that are usually quick to detect include:
- Frequent urination
- Excessive thirst
- Weight loss/weight gain
- Increased hunger
- Tiredness
- Lack of focus
- Numbness in the hands or feet
A group of eye problems can arise due to diabetes. Cataracts and glaucoma are only a couple of vision stealing side effects. If you have diabetes you may get cataracts at a younger age, and your chances of developing glaucoma doubles.
Early diagnosis of diabetes and maintaining a strict control of blood sugar and hypertension through a balanced diet, exercise and medication can help reduce your risk of developing eye disease that is associated with diabetes. Eye doctors are often the first to detect diabetes, so setting up annual appointments with your doctor can be life saving.
Preventing Eye Injuries at Home and the Workplace
Prevent Blindness America states that the most common agents of eye injuries in the workplace are:
• Flying objects (bits of metal, plastic and glass)
• Air or wind-blown objects (dust, wood and sand)
• Tools (screwdrivers, wrenches and etc.)
• Chemicals (oil, gasoline and acid)
• Harmful radiation (welding arcs and UV)
Prevent Blindness America (PBA) has estimated that 2.4 million eye injuries occur is the U.S. each year. About 1 million Americans have lost some degree of eyesight related to an eye injury. Experts say that wearing safety glasses or taking other common precautions can prevent or lessen the degree of more than 90% of these eye injuries.
At home, household cleaners and chemicals are the leading causes of eye injuries. The most common objects that cause the injuries besides chemicals and cleaners are:
• Mascara brushes and other cosmetic applications
• Fingernails (when applying and removing contact lenses)
• Lawn/Garden hand tools and machines
• Bungee cords
• Eyelash curlers
• Falls, bumping into walls, etc.
• Champagne corks
• Battery acid
• Toys/Games with hard/sharp edges
If there is a mishap you should contact your ophthalmologist immediately for
advice. Depending on the situation, your eye doctor may want you to flush your
eye/s with water or saline solution prior to your visit. He or she might also
recommend that you immediately go the hospital for further help. When working
with chemicals a sink should be near by at all times. If an accident occurs you should
flush your eyes with water for several minutes to dilute and rinse out any chemicals
that may have come into contact with your eyes.
Diagnosis and Treatment for Macular Degeneration
How is Macular Degeneration diagnosed?
When seeing an eye care professional, you should receive a comprehensive eye examination. This will perform a retinal examination to help diagnose macular degeneration. If a wet macular degeneration is detected or suspected a special test will be performed, which is called “fluorescein angiography”.
Many people ask, “What causes macular degeneration?” The answer is, there is no one certain thing that causes macular degeneration. However, there does appear to be certain risk factors, some of which include:
• Smoking
• Age
• Gender (women have a slightly higher risk)
• Family History
• High Cholesterol
• Caucasians – (are more like to have macular degeneration than African Americans)
• There are also suggestions that the following have been factors associated with increased risks: visible and UV light, low consumption of fruits and vegetables, light skin color and if you have blue eyes.
Can Macular Degeneration be treated?
Currently, there is no treatment for dry macular degeneration. However, if you have wet macular degeneration, there are intraocular injections that are the mainstay of treatment. Some of these are Avastin®, Lucentis® and Eylea®. One must know that vision that has already been lost may be restored in “some” patients, but not all. If vision cannot be restored, there are low-vision aids that exist that can help improve the quality of life.